Stereotactic Body Radiotherapy (SBRT) to your lung
This leaflet tells you about radiotherapy treatment to your lung called Stereotactic Body Radiotherapy (SBRT). It will explain how your treatment is planned and given. It will discuss side effects you may have and will tell you how to get more information and support. Contact telephone numbers are given at the end of the leaflet. We hope this leaflet answers your questions. Please ask us if you have other questions.
A glossary is provided at the front of this leaflet to help you understand any words that you may find unfamiliar.
Please bring a list of all the medication you are taking with the doses when you come for your radiotherapy treatment.
For more patient information is also available on Velindre website Please go to: https://velindre.nhs.wales/velindrecc/
Smoking is not allowed within the grounds and inside Velindre Hospital. If you need help giving up please ask us.
This information is evidence based and reviewed annually
Glossary of terms
CT Scanner - a machine that uses X-Rays to take detailed scans of your body
MRI Scanner - a machine that uses magnetism to take detailed pictures of your body
Treatment field - Each area that the treatment machine points to on your chest is called a treatment field.
Treatment Arc – a treatment method where the treatment machine moves around the couch in one or two circles (rotations) while giving treatment (one clockwise, the other anticlockwise)
Linear Accelerator or LA - The radiotherapy treatment machine where you will have your treatment (also called a LA or Linac). Each LA has a number e.g. LA1 or LA3
Wing board – a support with handles to keep you in position.
Vac bag – a support to lie on to help to keep you in position.
What is SBRT radiotherapy?
It is a type of radiotherapy treatment when higher doses are given over fewer treatment sessions to a precise area of your lung. These sessions are called fractions and each fraction is given on alternate days (Monday, Wednesday and Friday) for three, five or ten treatments. We give it this way because it reduces the effect of the radiation on your normal lung tissue. It also helps to reduce the risk of late side effects.
To make sure that your treatment is exactly right for you, you will first need to attend the Planning department.
After planning, your doctor will discuss with you whether SBRT radiotherapy will be the best treatment for you. If SBRT is not suitable, he or she will explain how your radiotherapy will be given.
Smoking during treatment
We strongly advise you to try to give up smoking. If you can, you will increase your chance of the treatment being successful. This would also be much better for your general health. Please contact the Information and Support radiographers or Stop Smoking Wales for advice (phone numbers page 14).
Planning your radiotherapy
To plan your radiotherapy you will need to have a CT scan. You will be asked to attend the Planning department which is at the front of Velindre hospital (parking is available). This scan gives your doctor a detailed picture of the area that needs treatment.
If you have already signed your consent form for treatment, you may only see your planning radiographers. They will explain everything that it going to happen to you.
If you have not signed your consent form, you will see your doctor at a later appointment. He or she will explain the benefits and risks of radiotherapy and will ask you to sign a consent form. Please discuss any problems or questions you may have before you sign the consent form.
We will need to inject a small amount of dye (called contrast) through a needle into your hand or arm before you have your scan. The dye helps to show the blood vessels and exact position of the area we need to treat. It should not cause any ill effects. However, please tell your planning radiographers if you have ever had a reaction to the dye when you have been scanned before.
We will ask you to undress to your waist and give you a gown to wear. We will ask you to take your arms out of the gown and will ensure your dignity by covering you up when ever possible. We will ask you to lie on a flat board (called a wing board) with handles to hold on to so your arms are above your head. You may be asked to lie on a ‘vac bag’. This will help you to stay in position. If you find your position uncomfortable please tell the radiographers as this is the position you will lie in throughout your treatment.
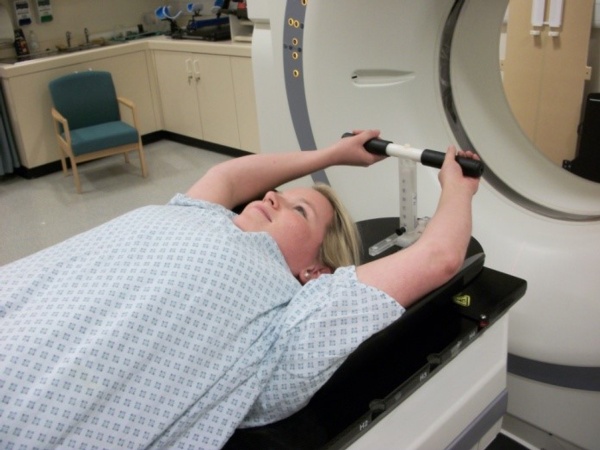 Staff member showing position lying on the wing board
Staff member showing position lying on the wing board
(you will need your gown off your shoulders)
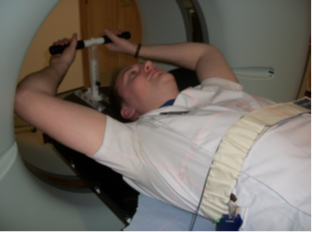 Staff member showing how the belt is worn
Staff member showing how the belt is worn
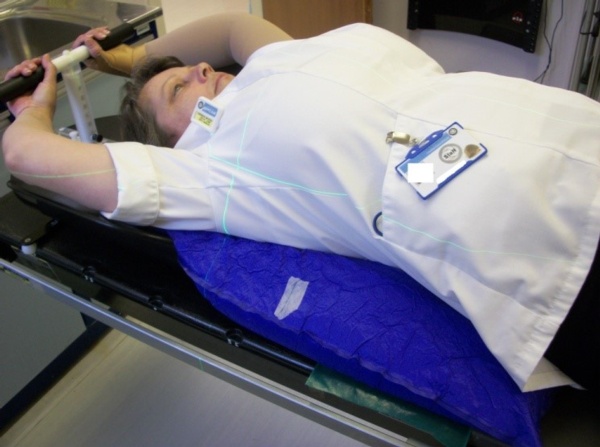 Staff member showing position on vac bag
Staff member showing position on vac bag
Your planning radiographers will place a special Velcro belt around your chest over the gown. A small monitor is put in the belt to look at your breathing during the scan. Your radiographers will ask you to breathe normally. This is important as they need to watch you breathe during your scan. After explaining everything to you, they will be quiet and not talk to you, to let you settle into your normal breathing.
You will not see or feel anything during the scan other than the couch moving gently. Your radiographers will leave the room to turn the scanner on, but they will be watching you very closely through a large window.
We will need to draw three marks on your skin which we will use as reference points for your treatment. It is helpful for us to permanently mark these reference points, and we will ask your permission before doing so.
We will make three tiny dots by using the tip of a sterile needle to place black ink just under your skin. It is a permanent mark but is as tiny as a freckle. This will mean we have accurate marks to position you for your treatment every day, so you are able to wash during treatment.
How long will it take?
It takes about 15-20 minutes to have your scan, but please allow an hour for your whole appointment.
When will I start treatment?
The scan images will be used to produce a treatment plan just for your needs. Treatment normally starts a few weeks after your planning appointment.
Starting your treatment
Please come to the back of the hospital to the radiotherapy entrance (parking is available). Give your name to the receptionist and she will show you where to wait. When you are called, your radiographers will show you where you can undress to your waist and put a gown on. Before each treatment we will ask you how you are feeling. Please tell us if you are having any problems before starting your treatment.
At each treatment visit, your radiographers will ask you to lie as you were for your CT planning scan. They will make sure you are as comfortable as possible. They dim the lights to adjust you into the exact position. Your treatment will be given as the machine moves around you. It will not touch you at all. Please breathe normally and keep as still as possible during your treatment,
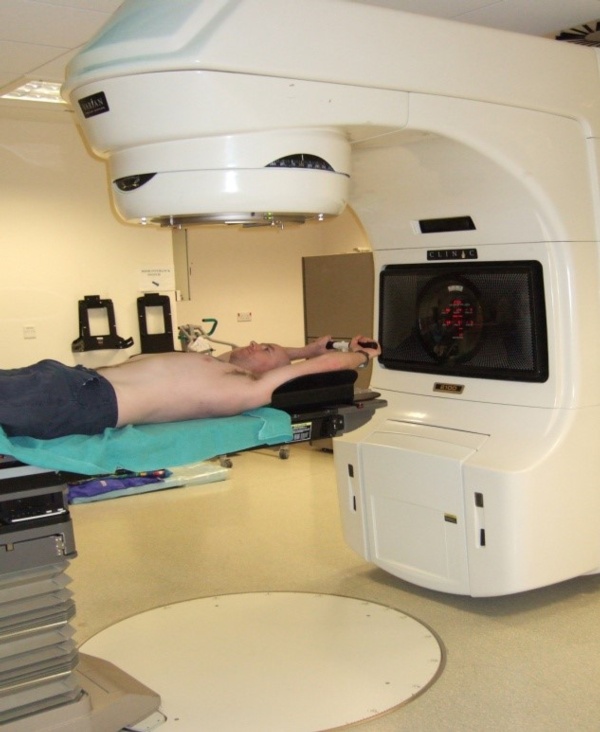 Treatment position on the treatment machine
Treatment position on the treatment machine
(You will be covered as much as possible)
Your radiographers leave the room to switch the machine on. The treatment is given from several (seven - ten) directions. Each direction is called a ‘field’ and each field will only take about one minute to treat. The radiographers will move the machine into each different position from outside the treatment room.
Or, your treatment can be given using one or two treatment arcs. An arc is a complete full circle of the machine. The machine can move clockwise and anticlockwise to deliver treatment. If two arcs are used, the machine will move anticlockwise and clockwise to give you your treatment.
Your radiographers will take images (pictures) of you before your treatment starts so this may take a little time before the machine starts giving you your treatment. These images show the exact position of your tumour as you breathe so your treatment will be in exactly the right place each day.
More images (pictures) may be taken during your treatment. Your radiographers will tell you if they are going to happen.
Your radiographers watch you carefully on television monitors. If you have any problems during the treatment, the machine can be switched off at any time. You will not feel anything when you are having your treatment, though you may hear the machine buzzing or beeping. Your treatment may take from 30 – 45 minutes.
Short term side effects of radiotherapy treatment
Tiredness
Radiotherapy can make you feel more tired than usual. You should listen to your body and rest if you need to. It is important to try to continue your normal activities during your treatment. Some people find a little exercise, drinking plenty of water and eating a healthy diet can help their tiredness.
Skin reactions
Your skin within the treatment area may become pink and warm, dry and itchy. We recommend using a mild soap (Dove or Simple soap) and moisturising your skin with aqueous cream.
Chest Pain
A few patients have some pain in their chest during treatment and for a few weeks after treatment. This is usually mild and should settle quite quickly.
Cough and Shortness of breath
Some patients notice an increase in their cough, shortness of breath and/or production of spit. This can contain blood, this is a normal reaction but please tell your radiographers if this happens.
Swallowing difficulties
Radiotherapy can cause your gullet (oesophagus) to become sore and inflamed. You may experience heartburn and indigestion. This could make eating and drinking uncomfortable. We can give you medication to help soothe this so that you can eat more easily.
Nausea and lack of appetite
You may feel sick or go off your food. We can give you anti-sickness tablets if you need it.
It is important to try to eat a healthy diet and drink more fluids during your treatment so that you do not lose weight. If eating becomes a struggle, it may help to eat several small meals a day than three main meals. We have dietitians available to see you who can give you advice on high calorie food and provide build up drinks to help you to keep your weight steady.
Long term side effects
Long term side effects are rare and do not happen to everyone. They can develop months or even years after the treatment has finished. Your doctor will discuss this with you. Please tell us if you have any concerns.
- The portion of your lung treated with radiotherapy may not work as well as before and you might notice a slight increase in breathlessness. This is due to scarring of the lung tissue (fibrosis) in and around the tumour area. If the rest of your lung works well then any symptoms you may notice will be very mild.
- If the tumour lies very close to a rib, the rib also receives a dose of radiotherapy and there is an increased risk of fracturing this rib in the future.
- Rarely, in a small number of patients, chest wall pain can occur and you may need pain killers.
- A very rare but potential effect is that radiation can cause tumours. If it does happen it is likely to be many years after treatment.
Remember, any of these small risks should be balanced against the problems of not treating the tumour with radiotherapy.
Follow up
We will arrange your follow up appointment to see your doctor at your last radiotherapy appointment. This appointment will be a few weeks after you finish your treatment. At your follow up appointments, your doctor will ask you about any side effects or symptoms that you have felt. Your doctor may arrange CT scans or X-rays at regular times.
Contact phone numbers
Information, support and review radiographers 029 2061 5888 ext 6421
Transport from Aberdare
Cancer Support Cynon Valley 01443 479369
Transport from Bridgend
Sandville 01656 743344
Transport from Merthyr
Cancer Aid Merthyr 01685 379633
Transport from Rhondda Cynon Taff
Community Cancer Services 01443 421999
Transport from Upper Rhymney Valley
CLURV (Bargoed) 01443 839326
‘Quit Smoking’ helpline 0800 0851 8800
0800 169 0169
Stop Smoking Wales 0800 085 2219
Helplines and website
Tenovus cancer support line 0808 808 1010
A charity supporting people with cancer and their families
Macmillan cancer support 0808 808 0000
www.macmillan.org.uk
A charity providing information about all aspects of cancer
Stop Smoking Wales 0800 085 2219
Roy Castle Lung Foundation 0800 358 7200
www.roycastle.org
A charity providing information and support for those affected by lung cancer
FS 37622
F.PI 38a Issue 2 Aug 12