Radiotherapy for gynaecological cancers
Radiotherapy for gynaecological cancers
What is radiotherapy?
Radiotherapy is a common treatment for cancer using high energy radiation, similar to x-rays. The type and amount of radiation that you receive will damage tumour cells, stopping them from dividing properly so they are destroyed. Healthy tissue is avoided where possible, however some healthy tissue is included which causes side effects.
It can be given either externally (external beam radiotherapy [EBRT]), internally (brachytherapy) or a combination of both. Radiotherapy can be given alone, after or instead of surgery. It can also be given with or after chemotherapy.
The number of treatments you have will vary depending on your diagnosis and stage. Radiotherapy is normally given Monday-Friday as an outpatient. You usually have 5 weeks of external radiotherapy. If you are also having brachytherapy (internal radiotherapy) too, this is given at the end of your external radiotherapy.
Your radiotherapy team
The doctor responsible for your care is called a Clinical Oncologist. They will prescribe and authorise your radiotherapy treatment. This will be planned by a team of physicists and planning radiographers. Therapy radiographers will deliver your radiotherapy.
Velindre is a teaching hospital so your team may include students in training. If you don't want a student present during your appointments, please tell us.
During radiotherapy you will be seen by the specialist review radiographers. They are able to advise you on how best to deal with any side effects, and can prescribe medication to help. They can provide information and advice on practical, financial, or emotional concerns you may have during your treatment. You can speak to them at any point during your treatment; their number is at the end of this leaflet.
Chemotherapy
Your doctor will discuss with you if chemotherapy is beneficial for you. If you are having chemotherapy, we will explain this part of your treatment and give you written information separately.
Hospital Transport
If you need hospital transport, please give us as much notice as possible to arrange this for you. There is a high demand for transport so you will need to be prepared to wait for some time to be picked up and taken home. Some local support groups can also arrange transport. Patients on particular benefits can claim travelling expenses, please ask when you come for your treatment.
Radiotherapy Planning
To plan your radiotherapy treatment accurately, you will need to have a CT scan. This scan will give your doctor a detailed view of the area that needs treatment. Please come to outpatients’ reception at the front of the hospital.
Your doctor will discuss the benefits and risks of radiotherapy and sign a consent form with you if you choose to go ahead with treatment. If you have already signed your consent form, you may only see the planning radiographers. They will explain everything that is going to happen to you.
The scan appointment usually takes about 20 minutes. Before you are scanned you are likely to be asked to do an enema and drink a few cups of water. This will be discussed with you when you arrive, you can eat and drink as normal prior to the appointment.
The scan will be done with you lying in the position you will need to be in for your treatment. We may ask you to remove your clothing but will give you a gown to wear. We will ask you to lie on the solid couch, with your arms across your chest. Please let the radiographers know if you are uncomfortable because you will need to keep this position, breathing normally, while we do the scan and for each day of your treatment.
During the scan, you will not see or feel anything. The radiographers will leave the room to turn the scanner on, but they will be watching you very closely through a large window.
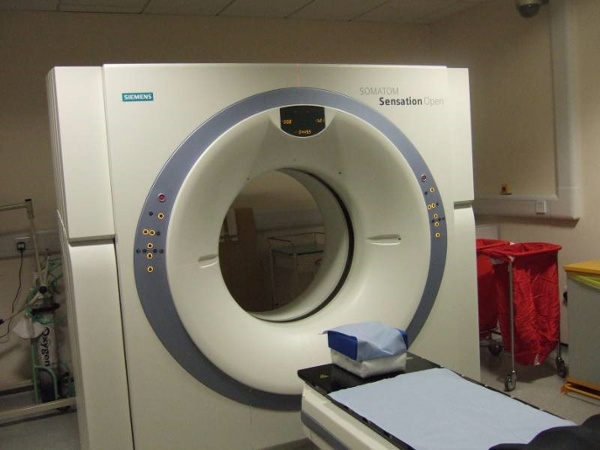
Picture of CT scanner
We may need to draw marks on your skin which we will use as reference points for your treatment. It is helpful to permanently mark these reference points, but we will ask your permission before doing so.
We make a tiny dot by using the tip of a sterile needle to place black ink just under your skin. It is a permanent mark but is as tiny as a freckle. This will mean we have accurate marks to position you for your treatment every day, so you are able to wash during treatment. Once this is done you can go home.
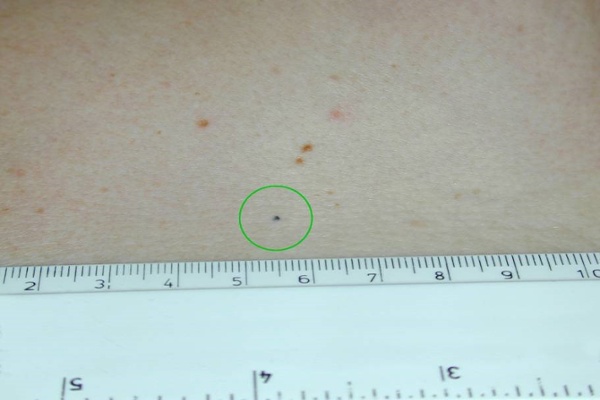
A picture of a permanent ink mark
Starting radiotherapy
There can be a few weeks between your planning scan and the start of your treatment. This is due to the time needed to plan your treatment and when the next available slot is on your treatment machine.
Please let us know if there is any time that you would be unable to come for treatment. We will try to take this in to account when we book your treatment. Please tell us if you have any special needs that may affect your appointments, such as hospital transport or other appointments such as chemotherapy.
We will send your first appointment in the post and will give you the rest of your appointments when you come for your first treatment.
Your first radiotherapy appointment
Please come to the radiotherapy reception at the back of Velindre hospital. Give your name and hand your letter to the receptionist. They will tell you where to sit and wait or direct you straight to your treatment machine.
If you are an in-patient, one of the hospital porters will collect you and take you to the treatment machine. You may be treated at any time in the day, depending on when there is a free slot on the treatment machine.
If you are due to have chemotherapy the same day as your radiotherapy, your chemotherapy will usually be given to you first then you will have your radiotherapy.
Your radiographers will talk to you before you go in for your first treatment. We will explain what will happen during your treatment and the possible side effects you may experience. We will also check when you completed your enema and drinking as this has to be timed carefully before treatment. Please ask us any questions you have about your treatment.
Occasionally unforeseen machine breakdowns can happen which may cause delays or rarely cancellation of your appointment on that day. We will explain this to you in more detail on your first day.
External radiotherapy is delivered by Linear Accelerators (shortened to LA or linac). They each have a number between 1 & 8. The linacs may look and sound different but they give the same treatment.
During external radiotherapy treatment
We will ask your name, address and date of birth every time you come for your radiotherapy treatment. In the treatment room, we will ask you to lie on the couch in the same position you were in for your planning scan. The radiographers will position you carefully using the permanent reference marks made at planning and move the machine around you. Once you are in the correct position, we will ask you to lie still and breathe normally.
The linac is controlled and moved by the radiographers outside the room. When the machine is moving, it may come close to you, but it will not touch you. When the machine is switched on you won’t see or feel anything, but you may hear the machine buzzing.
The radiographers will watch you carefully on cameras. If you need us during treatment please wave your hand. We can pause and restart the treatment if needed.
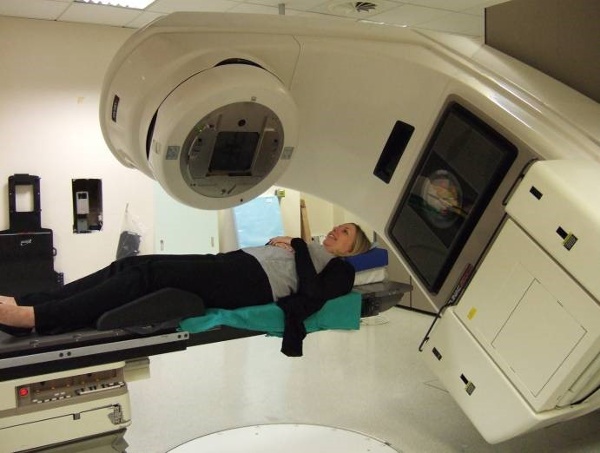
Picture of a linac machine
You will need to lie still on the treatment couch for about 10-15 minutes. The treatment itself (when you hear the buzzing noise) only takes a few minutes.
On your first day of treatment and at regular intervals through treatment, we will scan of the area that is being treated. You may be on the couch for a few extra minutes whilst this is done. The images are used to help us check you are in the correct position for your treatment. When your treatment finishes, the couch is raised so please stay still until the radiographers have lowered the couch. You can then get off and leave the treatment room.
Internal radiotherapy treatment (Brachytherapy)
After your external radiotherapy you may also have internal radiotherapy, known as Brachytherapy. Brachytherapy involves placing applicators in your uterus (womb), cervix and/or vagina. These are connected to a tiny radioactive source which gives a high dose of radiation to this area without damaging the surrounding healthy tissue. The machine that gives this treatment is called Flexitron.
If you have not had a hysterectomy the applicators are inserted in theatre, under general anaesthetic. Please read the section below.
If you have had a hysterectomy, you will not need to go to theatre or have an anaesthetic. Please skip to the vaginal vault section.
Your doctor will explain which treatment you will have.
Non-surgical patients (Theatre patients):
Before having your theatre sessions, you will need to have an MRI scan, a doppler scan and an anaesthetic assessment. These appointments will be given to you by the review radiographers. Theatre sessions are normally once a week on a Thursday.
Some patients are admitted onto the ward the night before each treatment. Others come into the ward early on the morning of treatment. You will continue to need regular blood tests. On the morning of your treatment the doctor will examine you and check your blood results and anaesthetic needs.
You are allowed solid foods and non-alcoholic drinks until midnight the night before your anaesthetic. Please tell the anaesthetic team about any medication you take, and they will advise you when to take your medication.
Theatre brachytherapy
In theatre you will be given a general anaesthetic before the procedure begins. Your doctor (Oncologist) will perform an internal examination and the treatment applicators are put into your uterus under ultrasound guidance. A catheter will be inserted into your bladder.
Once this is finished you will recover from the anaesthetic and have another MRI scan. You may be aware of the applicators inside you, and you may feel uncomfortable. If you are in any discomfort, please inform staff so that pain killers can be given.
The MRI scan is used by the doctors and physicists to plan your brachytherapy treatment. This can take a few hours, but you will be cared for on the ward while this is being done. You will be closely monitored during this time and pain relief can be given if needed. Once the plan is ready, you will be brought for brachytherapy treatment on your stretcher and will have light sedation after treatment for removal of the applicators and bladder catheter.
You will be taken back to the ward, for a period of rest before being allowed to return home, in most cases on the same day. It is important that another adult accompanies you home and is with you for 24 hours afterward. You should not drive a car operate machinery, or drink alcohol for 24 hours after a general anaesthetic.
Vaginal vault (non-theatre) brachytherapy
If you have had a hysterectomy, you will have brachytherapy without an anaesthetic. You will have either 2 or 5 treatments if external beam radiotherapy has been given. These will be on consecutive days. If you have not had external beam radiotherapy, you will have three brachytherapy treatments, once a week.
When you arrive for treatment, you may need to empty your bladder. You do not need to do any preparation for this treatment and can eat and drink as normal. You will need to remove your trousers and underwear, but a gown is provided to keep you covered. Once you are in the treatment room and are lying comfortably on the couch, your radiographer will do a gentle internal examination and then insert the treatment tube (similar to a plastic tampon). The tubes come in a range of sizes and insertion of the tube should not be painful for you.
Once the tube has been gently inserted into the vagina, it is then attached to the Flexitron unit, and the radiographers will leave the room to start treatment. The tiny radioactive source will travel from the Flexitron into the tube in your vagina and then back into the Flexitron. After treatment your radiographer will gently remove the tube and then you are able to change into your clothes and go home. The whole procedure will take about 20 minutes.
Brachytherapy treatment:
The radiographers connect the treatment applicator(s) inside you to the Flexitron unit. The radiographers will then leave the treatment room to switch the machine on and start your treatment. Once the treatment machine is switched on, the radioactive source will automatically travel into the applicator(s) to deliver your treatment.
You will not see or feel anything during your brachytherapy treatment but will hear a high-pitched buzz when treatment is being delivered. You will be watched by your treatment team on cameras focused on your head and shoulders throughout treatment. Once your treatment has finished, the radioactive source automatically returns to the Flexitron unit. Treatment time varies but is usually less than 20 minutes. Your treatment team will then enter the treatment room and remove the applicator(s).
After Brachytherapy Treatment:
You should not feel unwell, but you may notice some slight bleeding from your vagina and mild period-like cramps. After your treatment you are not radioactive but may be tired. If heavy bleeding develops then ring your GP or call the Velindre Treatment Helpline.
Side effects of external radiotherapy
Side effects normally start after about 2 weeks of treatment. Side effects only affect the area of the body that we are treating. Radiotherapy side effects can continue to build in your body for up to 14 days after you have finished your treatment. After 14 days you should start to feel better, but everybody’s recovery time is different.
Tiredness (fatigue)
Radiotherapy can make you feel more tired than usual. You should listen to your body and rest if you need to but continue your normal activities if you feel able. Some people find a little exercise and keeping hydrated can help their tiredness.
Diarrhoea
Radiotherapy to your pelvis may cause diarrhoea. We can give you advice and tablets to help manage this. Having diarrhoea can cause abdominal discomfort and pain. Please let us know if this occurs.
Urinary Incontinence
You may notice some urine leakage or difficulty controlling your bladder. Physiotherapy can sometimes help to manage this symptom. This can include being taught pelvic floor exercises, bladder re-training or being given simple advice about lifestyle changes. If you would like to be referred, please speak to a member of your health care professional team.
Cystitis (burning sensation when passing water)
Radiotherapy may irritate the lining of your bladder. This can make you feel you need to pass urine more often and it can burn. We will ask you to drink more water than usual to help keep your urine dilute. If the burning persists, please let the radiographers know.
Skin reactions
Your skin within the treatment area may turn pink, feel warm and tender or become dry and itchy. We encourage you to continue your normal skin care routine during treatment.
Menopausal symptoms
Radiotherapy can cause the onset of the menopause. You may have sweating (especially at night), hot flushes, irritability/mood swings, vaginal dryness, lack of sex drive and increased urgency in passing water. Please ask if you would like advice about controlling these symptoms.
Infertility
The radiotherapy will stop your ovaries from working so you will become infertile. Please speak to your doctor if you are concerned about this.
Vaginal dryness, narrowing and shortening (stenosis)
This may happen due to scar tissue developing in your vagina. Your vagina may become less flexible, making sex uncomfortable. Your review/brachytherapy radiographers will offer advice on using dilators to help with this, after you have completed all your treatments. Dilators are plastic tubes, like tampons, which you put into your vagina, as far as is comfortable for you, turn gently and take out. You use them in the privacy of your own home. If you would like more advice regarding these side effects, you can contact the specialist nurses for more help. See telephone numbers on the last page.
Longer term or permanent side effects
Although radiotherapy is carefully planned a small part of normal tissue will be treated. Although uncommon, it may cause long term symptoms such as:
· Diarrhoea
· Cystitis
· Bleeding from your bladder, vagina or back passage
· Recurrence of piles (hemorrhoids)
Please ask your doctor or radiographer if you want any more information about this.
Sex and radiotherapy
Treatment can cause narrowing, shortening or dryness of the vagina which may make sex uncomfortable. Using dilators regularly before resuming sex, and using a water-based lubricant for sex will reduce friction and help your comfort.
Some women feel able to continue having sex during treatment, others will feel too uncomfortable and not be ready. Everyone is different and it is important that you feel empowered to choose what is right for you.
If you have had a hysterectomy, it is recommended to wait six weeks before having sex. If you have had chemotherapy, it is recommended you use a condom during sex.
If you have questions about sex or would like to discuss it with someone, the review and brachytherapy radiographers or CNS nurses will be more than happy to help.
Don’t worry if you notice slight bleeding or spotting after sex. However, if bleeding is heavy or persists, please ask your team or treatment helpline for advice.
Follow up
Towards the end of your treatment we will give you an appointment for a follow up at a clinic with your doctor. This will usually be around 6 weeks after finishing your treatment and is over the telephone. Your second follow up, usually six weeks after the first) will be face to face. At this appointment, your doctor will give you a gentle vaginal examination. You may also have a blood test and an appointment for a scan. We will give you contact details for radiographers and nurses before you finish treatment. Please ring if you are worried about your side effects after you have finished treatment.
Patient information is available on Velindre website
Please go to: www.wales.nhs.uk/cancercentre
Smoking is not allowed within the grounds and inside Velindre Hospital. If you need help giving up please ask us or contact Stop Smoking Wales on 0800 085 2219.
Contact Phone Numbers
Velindre Treatment Helpline
029 2061 5888
Radiotherapy Booking Clerks
029 2019 6836
Radiotherapy Planning
029 2061 5888 ext 6150
Review Radiographers
029 2061 5888 ext 6421
Brachytherapy Radiographers
029 2061 5888 ext 6261
Velindre Theatre Office
029 2061 588 ext 2275
Gynae Nurse Specialists
029 2061 5888 ext 4679
Maggie’s Cancer Support
029 2240 8024
Macmillan Cancer Support
0808 800 0000
F.PI 24 Issue 16 July 2023